Desmopressin (DDAVP): what it treats and how to stay safe
Desmopressin — often called DDAVP — is a man-made hormone used when the body can’t hold on to water properly or needs a short boost in certain bleeding disorders. You’ll see it as a nasal spray, tablet, or injection. It’s effective, but it comes with real risks if used the wrong way. Here’s a clear, practical guide so you know what to expect and how to stay safe.
How desmopressin is used
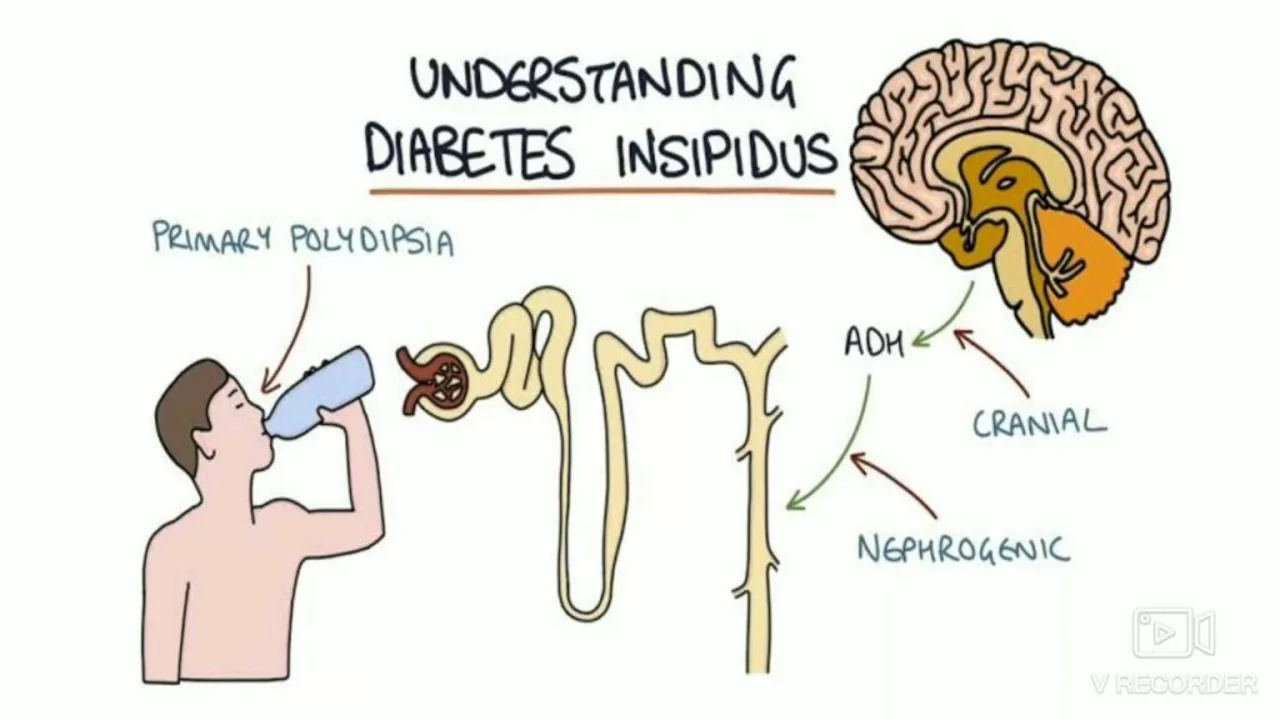
Doctors prescribe desmopressin mainly for three reasons: central diabetes insipidus (where the body loses too much water in urine), bedwetting (nocturnal enuresis) in some children and adults, and to help control bleeding in mild hemophilia A or certain von Willebrand cases. For diabetes insipidus it replaces a missing hormone to cut urine output. For enuresis it reduces nighttime urine. For bleeding disorders it helps release stored clotting factors briefly.
The form you get depends on the problem. Nasal spray is common for diabetes insipidus and enuresis. Tablets are used too. In hospitals, an injection may be used for bleeding control. Always follow the exact instructions from your prescriber — doses vary a lot by condition and patient.
Safety tips & monitoring — what really matters
Biggest risk? Hyponatremia (low blood sodium). Desmopressin tells the kidneys to hold water, so drinking a lot after a dose can dangerously dilute sodium. That can cause headache, confusion, nausea, seizures, even coma. Your doctor will usually ask you to limit fluids around the time you take a dose — follow that rule strictly.
Watch for warning signs: sudden severe headache, confusion, muscle cramps, vomiting, or seizures. If any of these appear, get medical help right away. For long-term use, your clinician will check blood sodium regularly, especially when starting treatment or changing dose.
Other common side effects include mild headache, facial flushing, nasal irritation with spray, and occasional abdominal discomfort. People with severe kidney disease, ongoing low sodium, or certain heart problems may be told not to use it.
Drug interactions and special cases: some antidepressants, antipsychotics, and other meds can increase the risk of low sodium when used with desmopressin. Tell your prescriber every medicine and supplement you take. Pregnant or breastfeeding people should discuss risks and benefits with their clinician — desmopressin is sometimes used but needs medical supervision.
Handling and buying: store nasal sprays at room temperature and keep tablets dry. Desmopressin needs a prescription — avoid buying from questionable online sellers. If you’re unsure about a pharmacy, check for a licensed contact or ask your doctor for reliable options.
Bottom line: desmopressin can be very helpful for specific problems, but it must be used carefully. Stick to your prescriber’s instructions, limit fluids when told, and get regular sodium checks when on long-term therapy. If something feels off, call your healthcare team right away.
As a blogger, I've recently come across a fascinating topic: Desmopressin and its role in managing post-transplant diabetes insipidus. For those who don't know, diabetes insipidus is a rare condition that causes excessive thirst and frequent urination. It turns out that Desmopressin, a synthetic hormone, has been found to be quite effective in treating this condition, particularly in patients who have undergone kidney transplants. The use of Desmopressin helps to regulate the patient's water balance and significantly improve their quality of life. It's always exciting to learn about new advancements in medical treatments and how they can make a difference in people's lives.
READ MORE