Cholesterol: What Your Numbers Mean and How to Lower LDL
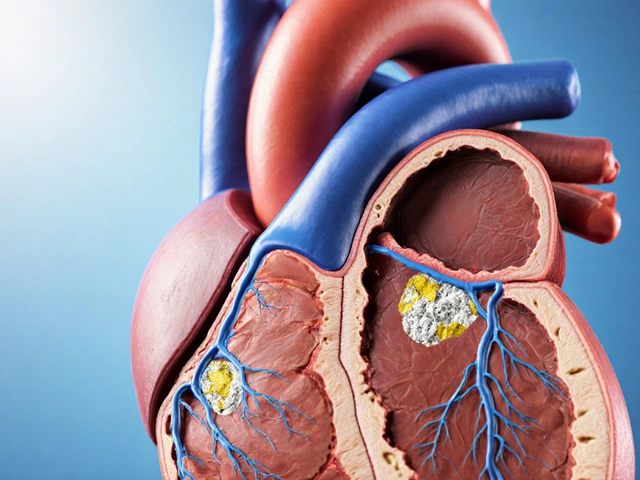
If your doctor told you your cholesterol is high, you probably want straight answers. Cholesterol isn't a disease by itself — it's a number that helps predict heart risk. The main targets are LDL (the 'bad' cholesterol), HDL (the 'good' cholesterol), and triglycerides. Knowing what those numbers mean gives you control.
Quick targets most providers use: LDL under 100 mg/dL is good for general adults, under 70 mg/dL if you already have heart disease. HDL should be higher (over 40 mg/dL for men, over 50 mg/dL for women). Triglycerides under 150 mg/dL is the usual goal.
Everyday steps that actually lower LDL
Food changes matter. Swap butter and hard fats for olive oil, avocados, and nuts. Eat fatty fish twice a week — salmon, mackerel, or sardines — to boost HDL and reduce triglycerides. Cut back on refined carbs and sugary drinks; they raise triglycerides and can lower HDL. Add soluble fiber: oats, beans, apples, and psyllium lower LDL by blocking cholesterol absorption.
Move more. Aim for 150 minutes of moderate aerobic activity each week (brisk walking, cycling, swimming). Strength training twice a week helps too. Even small gains — 20–30 minutes a day — improve your lipid numbers over months.
Lose weight if you need to. Dropping 5–10% of body weight usually lowers LDL and triglycerides and raises HDL. Smoking harms HDL and blood vessels — quitting helps within weeks. Limit alcohol: small amounts can raise HDL, but too much spikes triglycerides.
When lifestyle isn't enough: medicines and talking to your doctor
If lifestyle changes don't hit your targets or you have high risk for heart attacks, medications help. Statins are the most common and lower LDL reliably. Other options include ezetimibe, PCSK9 inhibitors, and bile acid sequestrants. Each has pros and cons and cost differences. Ask your clinician what target makes sense for your age and health.
Bring these questions to your next visit: What's my 10-year heart risk? What should my LDL goal be? Can we try diet and exercise first, and for how long? If I need a statin, what are the likely side effects and how will we monitor them? Are there interactions with my other meds?
Keep track. Repeat lipid tests as your doctor recommends — commonly 6–12 weeks after starting treatment, then every 3–12 months. If you take meds, report new muscle pain, unusual fatigue, or dark urine — your doctor may check liver enzymes or adjust dosing.
Bottom line: You can drop LDL with clear steps — smarter food choices, regular movement, weight loss, quitting smoking, and the right medicines when needed. Small, consistent changes make the biggest difference over time. If you're unsure where to start, ask your primary care provider for a simple plan you can follow for three months and then reassess with a repeat test.
Crestor, known by its generic name rosuvastatin, is one of the top-prescribed statins for lowering cholesterol. This article uncovers how Crestor works, who should use it, the pros and cons of long-term therapy, and real-life guidance for getting the best results. You’ll learn about its side effects, important stats, and useful health tips that actually make a difference for people using statins. Discover reasons why some people stick with it while others look for alternatives.
READ MORE