Post-Transplant Diabetes Insipidus: What It Is and What to Watch For
After a transplant you might suddenly pee a lot and feel very thirsty. That’s often diabetes insipidus (DI) showing up after surgery or as a reaction to drugs. DI isn’t the same as blood-sugar diabetes — it’s a water-balance problem. Left unchecked, it can cause dehydration, high sodium, and strain on your new organ. This page helps you spot DI fast and explains simple tests and real steps to get it under control.
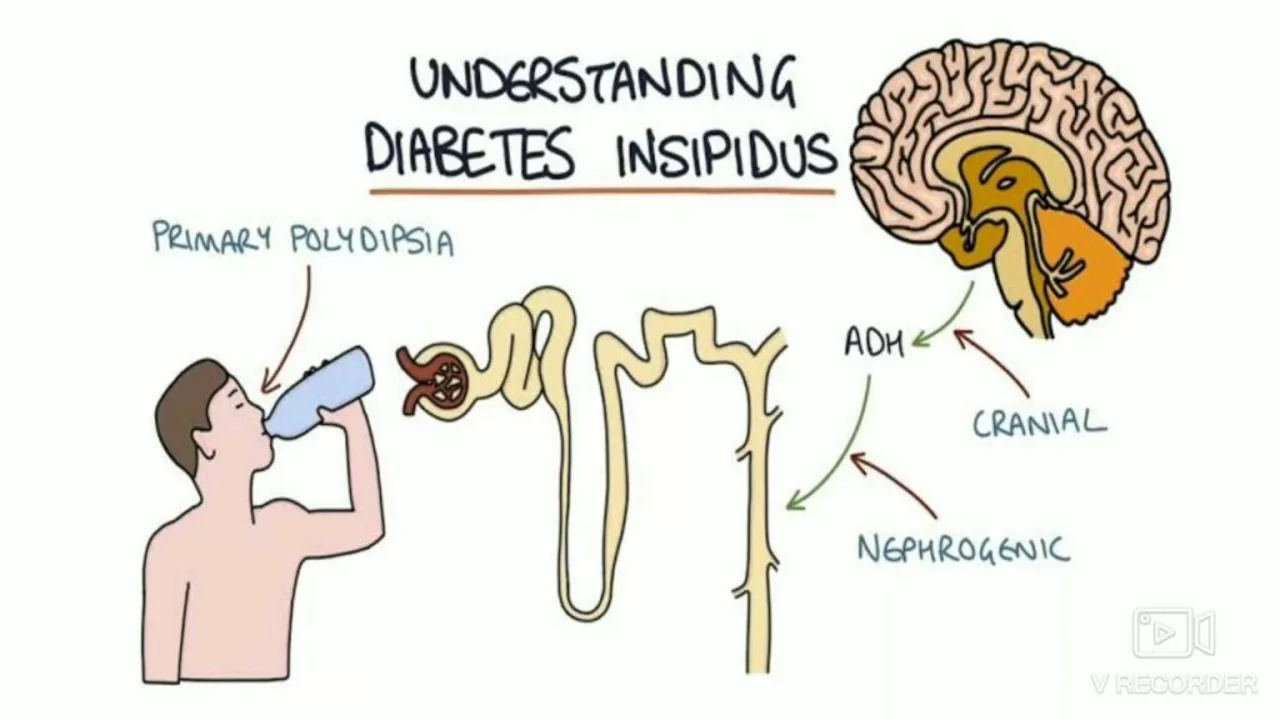
How DI Shows Up After a Transplant
Most common signs: urine output jumps (often several liters a day), urine looks very pale, you feel thirsty all the time, and you may get dizzy or weak. In transplant patients, DI can be short-lived (days to weeks) or last longer. Two main types appear after transplant: central DI, where the body makes too little ADH (the hormone that tells kidneys to keep water), and nephrogenic DI, where the kidneys don’t respond to ADH. Medicines like tacrolimus or cyclosporine — common after transplant — often cause the nephrogenic type.
Diagnosis — Simple, Practical Tests
If someone suspects DI, doctors usually check: how much urine you produce in 24 hours, urine osmolality (how concentrated urine is), and blood sodium. Typical findings: very high urine volume, low urine osmolality, and normal or high blood sodium. A quick check: give desmopressin (DDAVP) and see if urine concentration improves — if it does, it’s likely central DI; if not, it points to nephrogenic DI. After a transplant, doctors balance tests with the need to protect the new organ, so they may skip long deprivation tests and use targeted labs instead.
Treatment & Practical Management
First priority: stop dehydration. Drink free water if allowed, or get IV fluids in hospital. For central DI, desmopressin (nasal spray or injection) usually works well and quickly cuts urine output. For nephrogenic DI, the approach is different: doctors try to reduce or change the drug causing it (for example, lowering tacrolimus when safe), use a low-salt, low-protein diet to reduce urine volume, and sometimes give a thiazide diuretic which oddly reduces urine output. Nonsteroidal anti-inflammatory drugs (under close supervision) can also help in some cases. Don’t try medicine changes on your own—talk to your transplant team first.
Practical tips: measure and log urine output and fluid intake for your clinic; weigh yourself daily; avoid caffeine and alcohol (they make DI worse); keep scheduled blood tests to watch sodium and kidney function; and call your transplant center if urine output suddenly rises, you feel faint, or your lab shows high sodium. Most post-transplant DI cases can be managed safely with quick action and teamwork between you and your medical team.
As a blogger, I've recently come across a fascinating topic: Desmopressin and its role in managing post-transplant diabetes insipidus. For those who don't know, diabetes insipidus is a rare condition that causes excessive thirst and frequent urination. It turns out that Desmopressin, a synthetic hormone, has been found to be quite effective in treating this condition, particularly in patients who have undergone kidney transplants. The use of Desmopressin helps to regulate the patient's water balance and significantly improve their quality of life. It's always exciting to learn about new advancements in medical treatments and how they can make a difference in people's lives.
READ MORE